by Rinat Tal | Apr 25, 2024
A couple of weeks before the start of my M1 year at the University of Michigan Medical School (UMMS), I remember feeling a huge range of emotions. Of course, I was ecstatic to be coming to such an amazing “powerhouse” of an institution to finally start my medical education after three gap years. At the same time, I was anxious about leaving the city where I had built a community of mentors, role models and friends over seven years. I had also gotten used to having time to pursue my hobbies other than studying – what if I didn’t have time to bake or sing anymore in medical school?!
Once I arrived and got started, I quickly saw that although beginning a new chapter in life inevitably comes with some initial discomfort, UMMS is the perfect place for me to learn lessons from new people and experiences, build new relationships and continue to grow.
As far as finding mentors and role models is concerned, there is no lack of incredible physicians here who want to uplift medical students. As our first unit of the year got underway, I started reaching out to those in different fields of interest to explore all that’s out there (I’ve since learned that there is much more than I even knew existed!). I remember logging into a Zoom call in late September. Sitting in the virtual waiting room, I was nervous: What if the attending physician on the other side of the screen thought I was wasting her time? What if she thought my questions could have been answered with a Google search? However, she introduced herself and then immediately, cheerfully asked, “How can I help?” We spent the rest of the call discussing my interests, what life as a neonatologist looks like for her, opportunities to get involved in research and scheduling a time for me to come shadow in the NICU (neonatal intensive care unit) a few weeks later. After hanging up, I was both excited and overwhelmed by how many doors are open for medical students at UMMS. I was equally grateful that someone doing such important things and navigating such a busy schedule would take time out of her day just to “chat” with a first-year medical student who is trying to take full advantage of the next four years.

Had a great time learning more about Maternal-Fetal Medicine and shadowing Dr. Berman
While I was struck by this physician’s attitude and willingness to help, since that call, I’ve come to see that these conversations are not the exception but rather the norm at UMMS. I’ve had similar experiences with senior medical students and other attendings who have all been more than willing to help point me in the right direction. Since shadowing in the NICU, I also observed on the high-risk obstetrics floor of the hospital, in a fetal echocardiogram clinic, in the PICU (pediatric intensive care unit) and on a geriatrics consultation team.
During a conversation more recently, I was struck by the words of another physician, at the forefront of qualitative research in her field. She too was so willing to provide opportunities so that medical students can get involved in ways that are not only meaningful and personalized to their interests but will also help build them up for the future. When I expressed some insecurity because I don’t have much experience writing research papers intended for publication, she reassured me that with her and the team I would have the tools and learn the skills. I know she would have said the same thing to any student. I imagine she didn’t think there was anything unusual about the conversation, but it made me think even more about the community I’ve joined and the emphasis placed on opening doors for those coming up in their training.
The caliber of clinical role models and educators across the board is another reason I’m grateful for the opportunity to learn and grow here; I know that I will be a physician who thinks about all aspects of my patients’ lives and takes joy in getting to know them because I’ve had (and will continue to have!) examples who do the same. I’ve seen doctors make a conscious effort to empower their patients, diffuse tensions during difficult discussions and acknowledge when mental health needs must be met before delving into conversations about healthy habits and chronic disease risk.

Making holiday cookies with a fabulous group of American Medical Women’s Association mentors and mentees
I’m already becoming inspired by them and previous role models to help those who are currently applying to medical school and completing the pre-medical curriculum. Luckily for me, there are so many opportunities to begin practicing to be the type of mentor I want to be one day. As the undergraduate mentorship coordinator of our American Medical Women’s Association chapter, I periodically meet with my own mentees and plan events that provide some guidance for the pre-medical years and help foster connections between undergraduates and their M1 mentors. I’ve also loved speaking with students at my undergraduate institution who are interested in applying to UMMS.
As for the hobbies I worried I wouldn’t have time for, I’m happy to report that I’ve been able to continue them as a medical student and even picked up one more! To scratch my singing itch, I participate in a medical student a capella group, the Auscultations, and though I don’t act or dance, I’ve had many opportunities to watch my classmates perform in shows like The Smoker and Biorhythms. I’ve been able to keep baking, especially because of M-Home’s Flour Hour programming. And, at the encouragement of some friends in my class, I’ve taken up running and training for a half marathon (something I NEVER thought I would say about myself!). Because of the flexibility of our curriculum during the first year, I’ve had time to do these things while also staying in touch with friends and family in other states.
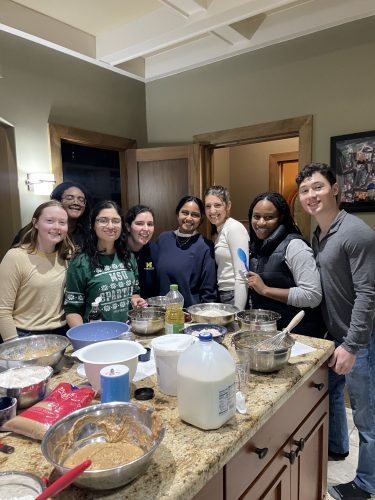
Baking muffins for our classmates at Flour Hour!
So, while I was initially apprehensive about leaving the comfort of a city I had grown to love, I now see that instead of leaving everything about it behind, I’m melding that stage of my life with my current experiences. I’m able to maintain those relationships and keep working with mentors from my gap years, even getting an academic paper published! At the same time, I’m making new connections and learning from incredible role models and classmates at UMMS. I know that these four years will foster personal and professional growth, and I can’t wait to see what kind of physician I become.
by Andrew Martinez | Apr 18, 2024

LMSA Midwest Conference
Growing up in a culturally diverse household, I’ve become intimately familiar with the joys of celebrating various holidays, savoring a wide range of cuisines, and traveling to my parents’ birth countries, which span opposite sides of the globe. I celebrate my diversity as it inspires me to foster linguistic and cultural competence in my future career as a physician. In college, I chose to study Spanish language and culture through my coursework, knowing this perspective would enable me to enrich my soon-to-come medical knowledge.
At the University of Michigan Medical School, I began my first year eager to engage with the Latinx medical community. I learned about the Medical Spanish program at Second Look (SL@M) and knew it would offer me the opportunity to integrate my background to better care for patients. The program, affiliated with the Latin American Native American Medical Association (LANAMA), has helped me find a community that spans all years at UMMS.

M1s, John Morse, Michella Parlett, and Ellie Wright (left to right) presenting their cultural presentation on La Paradoja Latina as part of the intermediate elective.
The Heart of Medical Spanish at UMMS
As the M1 Medical Spanish coordinator, the Intermediate Elective is the most common way students engage with the Medical Spanish program. Guided by Oliver Gatonez from Michigan Medicine Interpreter Services, this elective melds lectures with case-based discussions, history taking, and physical exam maneuvers, all in Spanish. Moreover, programming like cultural presentations and Spanish Standardized Patient experiences profoundly enriches our learning.
Casos Clínicos is another cornerstone of the program. These sessions facilitate discussions of clinical vignettes in Spanish, exploring cultural nuances crucial for treating Latinx patients. Led by Spanish-speaking faculty and residents, they allow for a deeper connection within the overarching Latinx community at Michigan Medicine. Most recently, we had the pleasure of hosting Bryan Figueroa, MD, a UMMS alum, who guided us through various neurosurgical medical cases, focusing on the treatment nuances for Latinx patients undergoing neurosurgery. All the while, we enjoyed homemade empanadas made by our very own Casos Clínicos coordinator, Stephanie Figueroa.
Our newest initiative, Horas Sociales, aims to bolster Spanish language proficiency and foster a sense of community among students at all language levels. Hosted in various informal settings, these gatherings encourage casual conversation and cultural exchange. Since founding Horas Sociales, we’ve nurtured a vibrant community of learners, eager to share and grow together.
I believe Medical Spanish is not only for those with a comprehensive background in the language but also enables everyone to gain cultural insights into a vast yet diverse population. My Cuban heritage from my father’s side is a fundamental aspect of my identity. My Spanish speaking might not be that of a native speaker, but over the years, it has transformed into a tool for connection that I use daily. It’s something I anticipate will only deepen as I start contributing to patient care in my upcoming clinical year.

LANAMA VP Alondra Alvarez and I at the LMSA Midwest Conference
Beyond UMMS: Connecting with the Latino Medical Community
My journey continued as I attended the LMSA Midwest Medical Conference with a group of my closest friends in February 2024. There was nothing better than stopping at one of the many coffee shops in Ann Arbor before we started our road trip to Case Western. This gathering was a vibrant celebration of Latinx culture in medicine, showcasing ongoing research and bringing together medical students, residents, and faculty from across the region. It was here, among peers from various backgrounds, that I grasped the broader impact of our work. The stories shared, the challenges discussed, and the research presented excited me for the everyday efforts to encourage and support Latinx communities both within and outside the medical field.
Natalie Vela, a graduating M4, led an incredible workshop on sustaining and starting Medical Spanish programs at medical schools in our region on behalf of the National Association of Medical Spanish (NAMS). She highlighted our program’s essential mission and the occasional challenges of such programming, including finding qualified long-term instructors and accreditation for the time students devote to this focus of their medical education. I hope to follow in her footsteps, as the outreach of this programming can expand across institutions and benefit a larger group of medical professionals and their patients.
A Call to Future UMMS Students
My journey through the Medical Spanish program at UMMS has been transformative, affirming my belief in the power of language concordance in healthcare. This program stands as a testament to Michigan and its students’ commitment to diversity, equity, and inclusion, offering a unique blend of clinical education and cultural immersion.
As I continue my medical school journey, I carry with me the lessons learned and the connections made, knowing they will shape my future in medicine. It’s a place where you can grow not just as a physician but as a compassionate and culturally aware human being. My commitment to my values has taught me that differences are made one patient, one conversation at a time.
by Joanna Hua | Apr 4, 2024
It took me two hours to find my DC Metro card. I had gone out of my way to get a special edition cherry blossom one during my gap years there, and I definitely still had money on it. I was excited to go back to a place that feels like a home and walk around with familiarity; the hotel where the conference was held was literally two blocks away from where I used to live.
 What I didn’t expect, however, was a flood of memories about my journey to medical school. Now that I was here as a visitor to present at a medical conference, I was passing through my old neighborhood as a medical student. The last time I had walked those streets was when I packed everything into my car and drove to Michigan to start this new adventure.
What I didn’t expect, however, was a flood of memories about my journey to medical school. Now that I was here as a visitor to present at a medical conference, I was passing through my old neighborhood as a medical student. The last time I had walked those streets was when I packed everything into my car and drove to Michigan to start this new adventure.
Here I was, living out my dream and more. It was so refreshing to remember the effort and passion that I poured into getting to this moment, especially in the midst of clinical rotations. Not only was I working towards the career of my dreams, I was also discovering new passions I never knew I had. The DC version of me would never have guessed that I would be interested in surgery and be presenting at a surgical conference.
Then I walked into the conference. I was immediately greeted by hundreds of people, all who looked like they just arrived at their old stomping grounds. People were greeting old friends they haven’t seen in a while, chatting excitedly about not only their research but a whole host of new developments in the medical forefront. I was fascinated by this microcosm but also suddenly intimidated. While I knew that this would be a new learning experience for me, I did not fully comprehend how daunting the barrier of entry would feel until then. With my surgery rotation under my belt, I was hoping to come in feeling at least a bit more prepared.
 In the face of my growing imposter syndrome, I was lucky enough to run into some familiar faces. The University of Michigan never disappoints with its representation – I was able to catch up with some M3s who I hadn’t seen since they disappeared for STEP studying and I disappeared into clerkships, chat with a few surgery residents who were excellent education fellows and update them on my growing interest in surgery, and feel supported by faculty, both familiar and new. It was such a relief to feel like I had a community, and it felt especially warm because my community was all in DC.
In the face of my growing imposter syndrome, I was lucky enough to run into some familiar faces. The University of Michigan never disappoints with its representation – I was able to catch up with some M3s who I hadn’t seen since they disappeared for STEP studying and I disappeared into clerkships, chat with a few surgery residents who were excellent education fellows and update them on my growing interest in surgery, and feel supported by faculty, both familiar and new. It was such a relief to feel like I had a community, and it felt especially warm because my community was all in DC.
The conference itself was a fantastic flurry of excitement. I was able to see developments that other medical schools and students were making in surgical research, support some of my friends in their incredible presentations, and spend some time chatting with the DaVinci robot rep to better understand the mechanics and try my hand at it myself. It was wonderful to reaffirm that I loved medicine and that I also loved to work with my hands. Even though my presentation was on the last day, my friends still showed up to cheer me on. I had an incredible time learning about surgery, honing my presentation skills, meeting new people, and growing into my UM community and the overall surgical field.
In hindsight, I realized by chatting with U-M people that I had been living right next to a “University of Michigan” bar in DC during my time here. I remember looking out my window and seeing random gaggles of people wearing Michigan gear and feeling a sense of pride and excitement after I found out I got into the medical school here. It turns out that my U-M community had been in DC all along – I just needed to find myself in it.
by Amanda Hernandez & Sharmi Amin | Mar 7, 2024
 As roommates and members of the Ethics Path of Excellence, dinners at our apartment often lend themselves to discussions of “hot topics” and ethical dilemmas. As curious medical students, we were eager to find a way to volunteer in the community and also share our knowledge as well as learn from others. As we explored avenues to do this, the Michigan High School Ethics Bowl fell onto our laps at the perfect time.
As roommates and members of the Ethics Path of Excellence, dinners at our apartment often lend themselves to discussions of “hot topics” and ethical dilemmas. As curious medical students, we were eager to find a way to volunteer in the community and also share our knowledge as well as learn from others. As we explored avenues to do this, the Michigan High School Ethics Bowl fell onto our laps at the perfect time.
The Michigan High School Ethics Bowl is an annually judged tournament that challenges high school students to think and discuss ethical cases. The Bowl, held at Greenhills School in Ann Arbor, is an opportunity for teams to present case studies to a panel of judges in a series of rounds. The cases are based on real-life situations and the students are tasked with deciding what should be done and be prepared to defend their decision. The winning team is eligible to compete in the National High School Ethics Bowl to represent the state of Michigan.
At the most recent Bowl, held in February, we served as a judge and a moderator for day one of the event. We arrived at Greenhills in the morning before the tournament began and watched the high schoolers nervously prepare for their day. Dressed up to the nines, the students looked focused and determined to argue their ethical dilemmas. We met our fellow judges and moderators with experiences ranging from OBGYN attendings to undergraduate ethic professors to ethical students to art collectors.
In the first case, students debated if simulating acts of torture in games like Legend of Zelda are inappropriate, and whether such actions make the game more violent than intended by its designers. One team argued that this type of “violence” may serve as an outlet for an internal aggression while another team debated that this may enable and inspire future violent acts in adolescents. The teams engaged in an organized debate, had the opportunity to be asked questions by the judges, and were scored based on intelligibility, focus, depth and judgment. After seven rounds of vigorous debate and competition, this year’s Bowl winner was Saline High School! This is Saline High’s first time winning the Hemlock Cup in their 11-year involvement in the tournament. A truly worthy feat!
The Ethics Bowl is just one of the engaging activities provided by the Ethics Path of Excellence. This extracurricular activity offers monthly sessions led by various Michigan faculty who are experts in bioethics. We’ve had the privilege of learning from Dr. Janice Firn, MD, who shared impactful ethics consult cases; Alethia Battles, JD, MSW, who discussed guardianship and the legal aspects of hospital ethics; and Drs. Naomi Laventhal, MD, MA, and Marin Arnolds, MD, who delved into neonatal ethics and the challenges of gestational viability. Beyond these enlightening lectures, Marisa Madrigal, our dedicated facilitator, keeps us informed about community ethics events, speaker sessions featuring bioethicists from around the country and writing opportunities.
I (Sharmi) was honored to present at the 2023 Michigan State Medical Society Bioethics Conference on the ethical implications of socioeconomic health disparities in pediatric post-traumatic brain injury care. This Path of Excellence has provided an incredible platform for connecting with fellow students and faculty from the Center of Bioethics and Social Sciences in Medicine (CBSSM). It gives us the opportunity to delve into challenging topics in health care and helps us develop the tools to navigate them. As roommates and fellow medical students, we enjoy sharing the Path experience and continuing to learn about ethics inside and outside the hospital together!
by Ellie Falahee | Feb 22, 2024
 Having always dreamt of going to medical school, I long imagined what my first days would look like: meeting my classmates in lecture, exploring the anatomy lab, and receiving my white coat. I never expected to start school in a tent in the woods, carrying my food and clothes on my back. However, through Creating Adventurous and Mindful Physicians (CAMP), I was able to spend my first few days of this new chapter surrounded by nature, bonding with my classmates, and feeling empowered and strong as I stepped out to fulfill my dream of becoming a physician.
Having always dreamt of going to medical school, I long imagined what my first days would look like: meeting my classmates in lecture, exploring the anatomy lab, and receiving my white coat. I never expected to start school in a tent in the woods, carrying my food and clothes on my back. However, through Creating Adventurous and Mindful Physicians (CAMP), I was able to spend my first few days of this new chapter surrounded by nature, bonding with my classmates, and feeling empowered and strong as I stepped out to fulfill my dream of becoming a physician.
Hailing from different colleges, states and past lived experiences, myself and ten other students met at an Ann Arbor park and were shuttled north to begin our adventure. Despite coming in as strangers, we quickly bonded as we divided up gear to carry in our backpacks and took turns reading the map to navigate as we hiked. Some of us were experienced backpackers, and others had never camped before, but regardless of background, we all shared the feeling of being in a new place with new people, excited and nervous to take on the next four years.
 Being heavily involved in Outdoor Education in undergrad, I recognize the special place that nature can be in bringing diverse groups of people together. There are few experiences that mimic the genuine joy of jumping into a lake at sunset, or gathering around a campfire to make s’mores. Nature creates an authentic space where you can show up as you are, offering opportunities that are both fun and challenging, but ultimately allowing for team-building, self reflection, and growth in a way that you can only find when you “unplug” from life outside of the woods.
Being heavily involved in Outdoor Education in undergrad, I recognize the special place that nature can be in bringing diverse groups of people together. There are few experiences that mimic the genuine joy of jumping into a lake at sunset, or gathering around a campfire to make s’mores. Nature creates an authentic space where you can show up as you are, offering opportunities that are both fun and challenging, but ultimately allowing for team-building, self reflection, and growth in a way that you can only find when you “unplug” from life outside of the woods.
 Choosing to start medical school “unplugged” from life back in Ann Arbor offered a chance to jump fully into this new chapter. One of the most meaningful moments on this trip for me was one night after we had finished hiking, sitting around the fire with my new friends. Our M2 and M4 leaders had passed out paper for each of us to write three of our biggest fears about starting medical school and a bowl to place the papers in when we were done. We all sat in silence for a bit as we reflected about what to write, and shyly placed each of our fears into the bowl. Then, our leaders began to anonymously read out each fear we’d written down. I remember being shocked that so many of the things I was nervous about were read four or five times, meaning other people had the same fears. “Everyone will be smarter than me” or “I won’t fit in” suddenly felt a lot less scary when I realized that I was not the only one who felt that way. Sitting under the starry sky in the Michigan wilderness, medical school suddenly felt a lot less intimidating, and I felt a lot less alone going into it.
Choosing to start medical school “unplugged” from life back in Ann Arbor offered a chance to jump fully into this new chapter. One of the most meaningful moments on this trip for me was one night after we had finished hiking, sitting around the fire with my new friends. Our M2 and M4 leaders had passed out paper for each of us to write three of our biggest fears about starting medical school and a bowl to place the papers in when we were done. We all sat in silence for a bit as we reflected about what to write, and shyly placed each of our fears into the bowl. Then, our leaders began to anonymously read out each fear we’d written down. I remember being shocked that so many of the things I was nervous about were read four or five times, meaning other people had the same fears. “Everyone will be smarter than me” or “I won’t fit in” suddenly felt a lot less scary when I realized that I was not the only one who felt that way. Sitting under the starry sky in the Michigan wilderness, medical school suddenly felt a lot less intimidating, and I felt a lot less alone going into it.
 Starting medical school with CAMP empowered me to feel at home at the University of Michigan Medical School, feel capable and confident in myself as I took this next step, and equipped me with new friendships that still build me up today. As I begin to wrap up my M1 year at Michigan, I now serve as the President of CAMP and am working with my incredible CAMP team to plan the next round of trips for our next class of students. As was my experience with CAMP, our goal is to create a safe environment for students to build confidence, make friends and feel at home at Michigan.
Starting medical school with CAMP empowered me to feel at home at the University of Michigan Medical School, feel capable and confident in myself as I took this next step, and equipped me with new friendships that still build me up today. As I begin to wrap up my M1 year at Michigan, I now serve as the President of CAMP and am working with my incredible CAMP team to plan the next round of trips for our next class of students. As was my experience with CAMP, our goal is to create a safe environment for students to build confidence, make friends and feel at home at Michigan.
Starting medical school is daunting, but starting medical school with new friends, new memories and a renewed confidence in yourself and your abilities can make the transition as seamless as possible. I am so grateful for the ways CAMP has made me feel welcome at Michigan Med and so excited to help create the same experiences for students who come after me!

Students from my CAMP group celebrating at our White Coat Ceremony!
by Krupa Patel | Feb 1, 2024
Before coming to the University of Michigan Medical School, I spent three years building the nonprofit organization, Lunar Doula Collective (LDC). After noting the lack of reproductive grief care at multiple health care systems, I helped build the first and only pregnancy loss doula program in Michigan. Not only did this experience inspire my motivation to pursue medicine, but it gave me a community that shared my passion for social justice and health equity.

2023 LEAD Cohort at Adventure Leadership in the summer
As I prepared to transition into medical school, I remember feeling anxious about leaving LDC behind. This next chapter of my life would come with a lot of challenges: making new friends, figuring out work-life balance and adjusting to a different environment. While I felt excited and grateful to begin my journey, I was equally as nervous to navigate this process as a first-generation medical student.
When I heard about the LEAD (Leadership and Enrichment for Academic Diversity) Pre-Matriculation Program, I knew right away that I wanted to apply. This two-week leadership course is thoughtfully designed to prepare and help transition incoming medical students. Through early exposure to resources and mentorship, LEAD students are empowered to cultivate change in the community and seek professional growth.

All smiles at our White Coat Ceremony – July 23, 2023
During my time in LEAD, I heard from faculty and current students about their experiences at UMMS as they shared advice on how to navigate medical school. From learning effective study strategies to identifying research opportunities, I began growing more confident as the first day of class approached. LEAD programming also included team bonding activities, health equity lessons and stress management strategies. As part of the LEAD cohort, I truly felt like I had the resources, attributes and support system to succeed.
Another thing I appreciate about LEAD is the longitudinal educational enrichment. Our cohort continues to meet throughout the year to hear from various guest speakers and engage in professional development opportunities. Whether it’s a financial literacy seminar or a CV-building workshop, we get to collectively decide what events and topics would interest and benefit us the most. At the end of LEAD, I got paired with a senior medical student as part of a peer-mentoring program. Having someone to lean on and seek guidance from was so immensely helpful when I began medical school.

Checking out the Big House Stadium with some LEAD friends!
What surprised me the most about LEAD was its unique culture of collaboration and connectedness. I found a safe space to talk about failures, learn from my peers, and explore diverse perspectives. This close-knit community has been my source of encouragement and inspiration throughout my M1 year. I’ve seen my LEAD peers represent our class on the Student Council, encourage community building through M-Home, and facilitate resource and knowledge-sharing. Taking what I learned from LEAD, I was personally inspired to start two new organizations for medical students at UMMS this year: The Ruth Jackson Orthopaedic Society Chapter and Medicine in Motion.

LEAD Besties: Krupa Patel (left) and Jennifer Lee (right)
The LEAD Program was the perfect start to my medical school journey. It allowed me to strengthen my leadership and professionalism skills, value the diversity and experiences of my peers, and turn my doubts and fears into self-confidence. These are lessons I will carry with me throughout and beyond the next four years. I am grateful to the Office of Admissions, the Office for Health Equity and Inclusion (OHEI), and the Office of Medical Student Education (OMSE) for planning and hosting such an impactful experience. To my 2023 LEAD cohort: thank you for our little community that cheers each other on, dreams big, and makes UMMS feel like home.


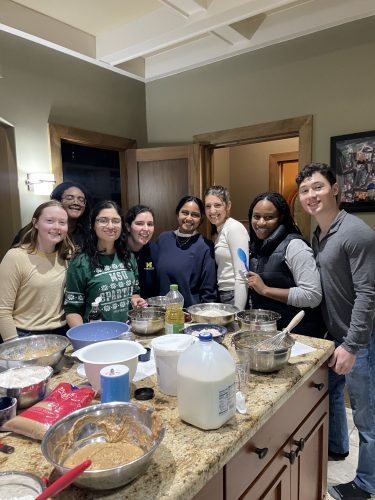





 What I didn’t expect, however, was a flood of memories about my journey to medical school. Now that I was here as a visitor to present at a medical conference, I was passing through my old neighborhood as a medical student. The last time I had walked those streets was when I packed everything into my car and drove to Michigan to start this new adventure.
What I didn’t expect, however, was a flood of memories about my journey to medical school. Now that I was here as a visitor to present at a medical conference, I was passing through my old neighborhood as a medical student. The last time I had walked those streets was when I packed everything into my car and drove to Michigan to start this new adventure. In the face of my growing imposter syndrome, I was lucky enough to run into some familiar faces. The University of Michigan never disappoints with its representation – I was able to catch up with some M3s who I hadn’t seen since
In the face of my growing imposter syndrome, I was lucky enough to run into some familiar faces. The University of Michigan never disappoints with its representation – I was able to catch up with some M3s who I hadn’t seen since  As roommates and members of the
As roommates and members of the  Having always dreamt of going to medical school, I long imagined what my first days would look like: meeting my classmates in lecture, exploring the anatomy lab, and receiving my white coat. I never expected to start school in a tent in the woods, carrying my food and clothes on my back. However, through
Having always dreamt of going to medical school, I long imagined what my first days would look like: meeting my classmates in lecture, exploring the anatomy lab, and receiving my white coat. I never expected to start school in a tent in the woods, carrying my food and clothes on my back. However, through  Being heavily involved in Outdoor Education in undergrad, I recognize the special place that nature can be in bringing diverse groups of people together. There are few experiences that mimic the genuine joy of jumping into a lake at sunset, or gathering around a campfire to make s’mores. Nature creates an authentic space where you can show up as you are, offering opportunities that are both fun and challenging, but ultimately allowing for team-building, self reflection, and growth in a way that you can only find when you “unplug” from life outside of the woods.
Being heavily involved in Outdoor Education in undergrad, I recognize the special place that nature can be in bringing diverse groups of people together. There are few experiences that mimic the genuine joy of jumping into a lake at sunset, or gathering around a campfire to make s’mores. Nature creates an authentic space where you can show up as you are, offering opportunities that are both fun and challenging, but ultimately allowing for team-building, self reflection, and growth in a way that you can only find when you “unplug” from life outside of the woods. Choosing to start medical school “unplugged” from life back in Ann Arbor offered a chance to jump fully into this new chapter. One of the most meaningful moments on this trip for me was one night after we had finished hiking, sitting around the fire with my new friends. Our M2 and M4 leaders had passed out paper for each of us to write three of our biggest fears about starting medical school and a bowl to place the papers in when we were done. We all sat in silence for a bit as we reflected about what to write, and shyly placed each of our fears into the bowl. Then, our leaders began to anonymously read out each fear we’d written down. I remember being shocked that so many of the things I was nervous about were read four or five times, meaning other people had the same fears. “Everyone will be smarter than me” or “I won’t fit in” suddenly felt a lot less scary when I realized that I was not the only one who felt that way. Sitting under the starry sky in the Michigan wilderness, medical school suddenly felt a lot less intimidating, and I felt a lot less alone going into it.
Choosing to start medical school “unplugged” from life back in Ann Arbor offered a chance to jump fully into this new chapter. One of the most meaningful moments on this trip for me was one night after we had finished hiking, sitting around the fire with my new friends. Our M2 and M4 leaders had passed out paper for each of us to write three of our biggest fears about starting medical school and a bowl to place the papers in when we were done. We all sat in silence for a bit as we reflected about what to write, and shyly placed each of our fears into the bowl. Then, our leaders began to anonymously read out each fear we’d written down. I remember being shocked that so many of the things I was nervous about were read four or five times, meaning other people had the same fears. “Everyone will be smarter than me” or “I won’t fit in” suddenly felt a lot less scary when I realized that I was not the only one who felt that way. Sitting under the starry sky in the Michigan wilderness, medical school suddenly felt a lot less intimidating, and I felt a lot less alone going into it. Starting medical school with CAMP empowered me to feel at home at the
Starting medical school with CAMP empowered me to feel at home at the 



